HbA1c or Glycated Haemoglobin is a term known to almost all Indians, thanks to the high prevalence of diabetes not only in their direct family but also in their community. Be it a healthcare worker or a member of the general public, I can surely say that you must know a diabetes patient personally, may it be your friend, family or a loved one.
HbA1c is widely used as a diagnostic and monitoring method for diabetes in general. Even with the availability of other tests like OGTT, FBS, PPBS, it still remains the preferred mode of classifying people into diabetics and non-diabetics. This is perhaps due to the following advantages:
- No fasting required
- Depicts the trend of the previous 2-3 months
- Adopted in guidelines [WHO, ADA]
However, depending on HbA1c as the sole criteria for diagnosis and monitoring of diabetes can lead to the misinterpretation, specially in Indian populations. This effect is seen due to the enormous burden of haematological abnormalities [IDA], genetic factors [G6PD deficiency], social and metabolic influences.
The Article “The limitations and fallacies of relying on glycosylated haemoglobin for diagnosing and monitoring diabetes in Indian population” highlights the discordance between HbA1c and blood glucose levels, with a special focus on people with altered erythrocytic dynamics.
My article tries to describe all of it in a much simpler way, so that you can digest the information easily and also get to know about medical topics, without obsessing over the minute details.
Special thanks to Shambik Sir [my Physics teacher] for telling me about this article published in The Lancet Regional Health – Southeast Asia, 2026.
Join Weekly Health Newsletter
Every week, I will share with you information about Natural Health, Diet, Exercise, Yoga & Wellness.
STRUCTURE OF THE STUDY
Search Terms
- HbA1c
- glycated haemoglobin
- diabetes
- diagnosis
- oral glucose tolerance test (OGTT)
- iron deficiency anaemia
- hemoglobinopathies
- G6PD deficiency
- Polycythaemia
- erythrocyte lifespan
- South Asians
- India
Filters
To select
- observational studies
- randomized controlled trials
- meta-analyses
- national survey reports
- clinical guidelines
Grouping
HbA1c as a :
- Diagnostic tool [Compared to OGTT, FBS]
- Monitoring marker [Compared to SMBG, CGM, Fructosamine, Glycated albumin]
Selection Criteria
If they provided data on
- Discordance between HbA1c and glucose-based indices
- Diagnostic or monitoring performance in the presence of hematologic disorders
- Alternative biomarkers such as fructosamine, glycated albumin, or 1,5-anhydroglucitol.
Special Emphasis
On studies focused on the effect of haematological conditions on HbA1c.
HbA1c AND BLOOD GLUCOSE
Blood Test for HbA1c
HbA1c is hailed as the gold standard test for assessment of glycaemic control. It is used for the diagnosis of prediabetes and diabetes. This choice can be attributed to:
- Convenience [no fasting]
- Stability before analysis
- Relatively low variation among individuals
The American Diabetes Association guidelines give the following cut-offs for classification of diabetes :
- < 5.7% : Normal
- 5.7 to < 6.5% : Prediabetes
- > 6.5% : Diabetes
On the other hand, here’s what WHO says about it :
- HbA1c can be used as a diagnostic test for diabetes if stringent quality assurance tests are in place and assays are standardized to criteria aligned to the international reference values, and there are no conditions present which preclude its accurate measurement.
- An HbA1c of 6.5% is recommended as the cut point for diagnosing diabetes.
- A value of less than 6.5% does not exclude diabetes diagnosed using glucose tests.
- Quality of evidence assessed by GRADE: moderate
- Strength of recommendation based on GRADE criteria: conditional
In short, it has pointed out the specific requirements, only under which the credibility of the test is assured.
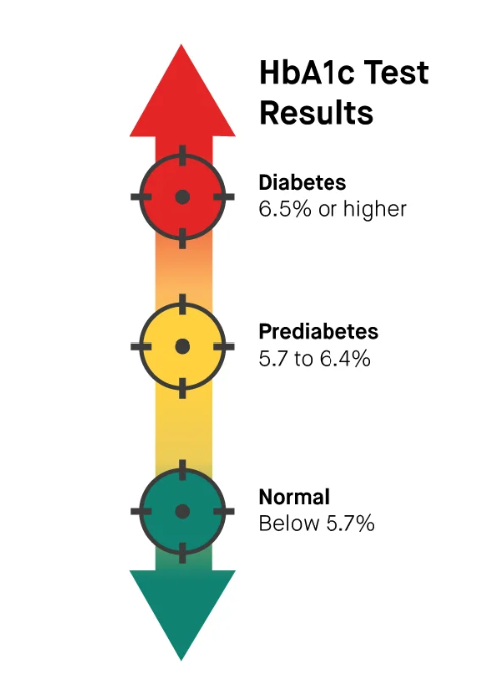
American Diabetes Association Guidelines
In the Indian scenario, these are quite often overlooked, thus simplifying and increasing the “efficiency” of the diagnostic and monitoring process. It leads to either misdiagnosing or overdiagnosis of diabetes, hindering the treatment plan, prolonging the latent period, and increasing the risk of complications like diabetic neuropathy, retinopathy, etc.
When the HbA1c and mean glucose concentrations were compared using various methods like Continuous Glucose Monitoring Systems [CGMS], Fasting Plasma Glucose, Self-Monitoring of Blood Glucose, a discordance was observed between them. The causes of the variations are individually discussed in the upcoming topic.
So, to remove such variations, the researchers proposed 2 related indices.
- Glycation Gap [GGap] : Predicted HbA1c from plasma fructosamine – Measured HbA1c
- Haemoglobin Glycation Index [HGI] : Measured HbA1c – Predicted HbA1c from fasting plasma glucose level
CAUSES OF DIVERGENCE IN INDIA
Four major causes are underlined in the paper. They are :
- Haematological Abnormalities
- Standardisation of Assays
- National Glyco-haemoglobin Standardisation Programme
- Seasonal variation
Haematological Abnormalities
Here, a table was provided with different causes and their underlying mechanisms. In short, it talks about three cases in general:
FALSE LOW HbA1c
Due to the following causes, RBC lifespan decreases, thus decreasing the time it gets for glycation of Haemoglobin.
- Haemolytic anaemia
- G6PD deficiency (subclinical haemolysis)
- Acute blood loss (increased young RBCs)
- Pregnancy (increased RBC turnover, haemodilution)
- Chronic liver disease (hypersplenism, bleeding)
- Chronic renal failure (Decreased RBC survival)
- Recent blood transfusion (dilution effect)
- High-dose vitamin C (assay interference / Decreased glycation)
FALSE HIGH HbA1c
It is opposite to false low HbA1c. Here, the lifespan increases, thus increasing glycation time.
Iron deficiency anaemia (IDA) (Increased glycation, prolonged RBC life)
Polycythaemia (prolonged RBC lifespan)
UNRELIABLE OR VARIABLE HbA1c
It is due to a mix of the mechanisms or because it interferes with the assay.
- Hemoglobinopathies (variant & method dependent)
- Chronic renal failure (carbamylated Hb interference)
- Alcohol abuse
- Liver disease
- High BMI (obesity)
- Race/ethnicity differences (e.g., South Asians, African origin)
- Elderly (RBC morphology changes)
- Recent transfusion
- Hypertriglyceridemia, hyperbilirubinemia
- Lead poisoning
- Drugs: opioids, salicylates, ribavirin, vitamin E
- Asplenia
- Assay variation
- Seasonal variation (noted in Indian population)
In India, we see high rates of IDA (affecting an estimated 25%–68% depending on age, sex, and study region), hemoglobinopathies ((0.37%-5.9%), with regional and ethnic variation), and G6PD deficiency (7.7–8.5% with high prevalence in tribal group).
G6PD deficiency alone resulted in a median delay of 4.1 years in diabetes diagnosis and a 37% increase in microvascular complications.
Standardisation of Assays
Many laboratories use methods other than High-performance liquid chromatography (HPLC) for the assessment of HbA1c. Even ion-exchange HPLC, which is widely employed in Indian labs, may yield uninterpretable results in individuals with silent haemoglobin variants.

National Glyco-haemoglobin Standardisation Programme
A survey of 310 Indian laboratories found that 75% used HbA1c for diabetes mellitus diagnosis, but only 70% of these assays were National Glyco-haemoglobin Standardization Programme (NGSP)- certified. It shows the possibility of gaps in quality assurance between different labs throughout India.
Thus, the labs need to adopt standardised NGSP-certified HbA1c methods for better diagnosis.
Seasonal Variations
HbA1c levels are highest during the monsoon (June–September) and lowest during autumn (October–November). In patients with well-controlled diabetes, HbA1c tends to rise during winter and the monsoon. However, in patients with HbA1c ≥ 6.5%, levels tend to decrease during the monsoon and autumn.
OTHER APPROACHES
To assess glycemia, we can adopt alternative and complementary approaches as listed below.
- Self-Monitoring of Blood Glucose [SMBG]
- Fructosamine
- Continuous Glucose Monitoring
- Flash Glucose Monitoring
- Glycated Albumin
- 1,5-Anhydroglucitol
- Haemoglobin Glycation Index
Self Monitoring of Blood Glucose
CLINICAL & POLICY IMPLICATIONS
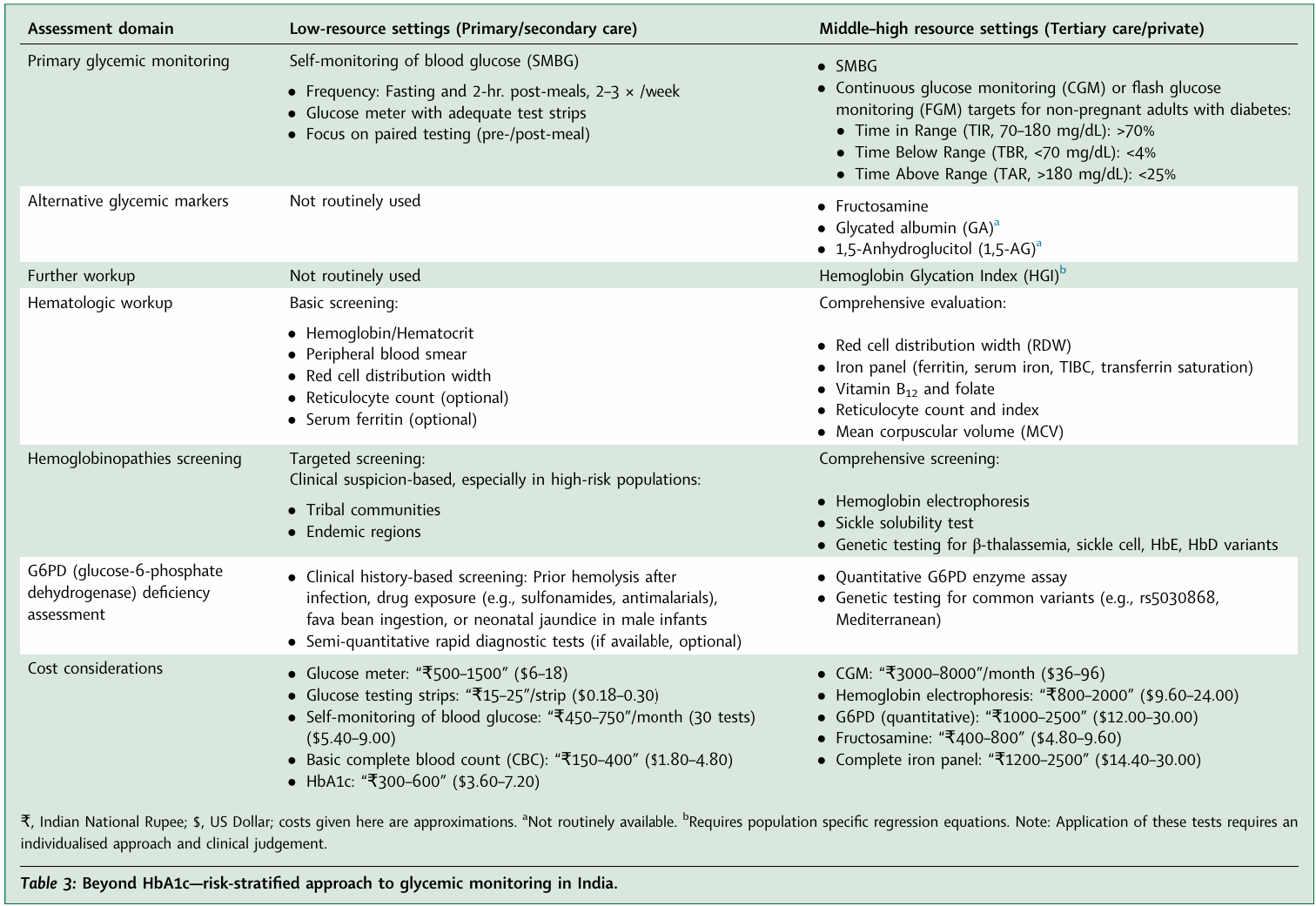
For Diagnosis
Standardised OGTT as Gold Standard
For Monitoring
- HbA1c (measured using a standardized and NGSP-certified assay) should be interpreted
- With serial fasting and postprandial blood glucose values.
- CGMS if affordable and available.
REFERENCE
The limitations and fallacies of relying on glycosylated hemoglobin for diagnosing and monitoring diabetes in Indian populations. Samajdar, Shambo Samrat et al. The Lancet Regional Health - Southeast Asia, Volume 45, 100724
Use of Glycated Haemoglobin (HbA1c) in the Diagnosis of Diabetes Mellitus. Abbreviated Report of a WHO Consultation. WHO/NMH/CHP/CPM/11.1

0 comments