The WHO’s Global Antimicrobial Resistance Surveillance System (GLASS) report highlights a sharp increase in antibiotic resistance, particularly in low- and middle-income nations such as India, where healthcare systems are often fragile.
Drawing on data from more than 23 million bacterial infections reported in over 100 countries, the report reveals that between 2018 and 2023, over 40% of antibiotics have become ineffective against common infections of the bloodstream, urinary tract, digestive system, and reproductive organs.
In 2021 alone, bacterial infections caused an estimated 7.7 million deaths globally, with drug resistance contributing to 4.71 million of those and directly causing 1.14 million fatalities.
This article delves deeper into the topic of antimicrobial resistance and its current effects worldwide and in India.
Join Weekly Health Newsletter
Every week, I will share with you information about Natural Health, Diet, Exercise, Yoga & Wellness.
INTRODUCTION
Antimicrobial resistance (AMR) is emerging as one of the most serious challenges to global health, weakening the power of critical medicines and increasing the danger posed by infections that were once easily treatable, as well as by routine medical procedures.
Through its Global Antimicrobial Resistance and Use Surveillance System (GLASS), the World Health Organization (WHO) helps nations establish robust surveillance systems and produce comparable data that can drive informed public health policies.
On 13 October 2025, WHO published Global antibiotic resistance surveillance report 2025, which offers a comprehensive global picture of antibiotic resistance patterns, drawing on evidence from more than 23 million confirmed cases of bloodstream, urinary, gastrointestinal, and urogenital infections (including gonorrhoea). The findings are based on data submitted by 104 countries in 2023 and 110 countries over the 2016–2023 period.
If you'd like to understand what AMR [Antimicrobial Resistance] is, then please look at this article. The following is a synopsis of the detailed analysis provided by WHO.
AT A GLANCE

Since the launch of GLASS in 2016, antimicrobial resistance (AMR) data have been submitted by 110 countries, including three territories and regions. Participation has expanded significantly—from just 25 countries in 2016 to 104 in 2023, reflecting a growth of more than 300%.
The steady increase in reporting underscores the growing global recognition of the importance of sharing surveillance data as a collective public health responsibility. Despite these improvements, considerable gaps in data availability and reporting continue to hinder a complete global picture.
In 2023, antibiotic resistance was detected in roughly one out of every six laboratory-confirmed bacterial infections worldwide. The highest resistance levels were found in urinary tract infections (1:3 cases) and bloodstream infections (1:6).
Lower resistance rates were observed in gastrointestinal infections (1:15) and urogenital gonorrhoeal infections (1:125).
Trends of AMR: median annual change in percentage, 2018–2023.
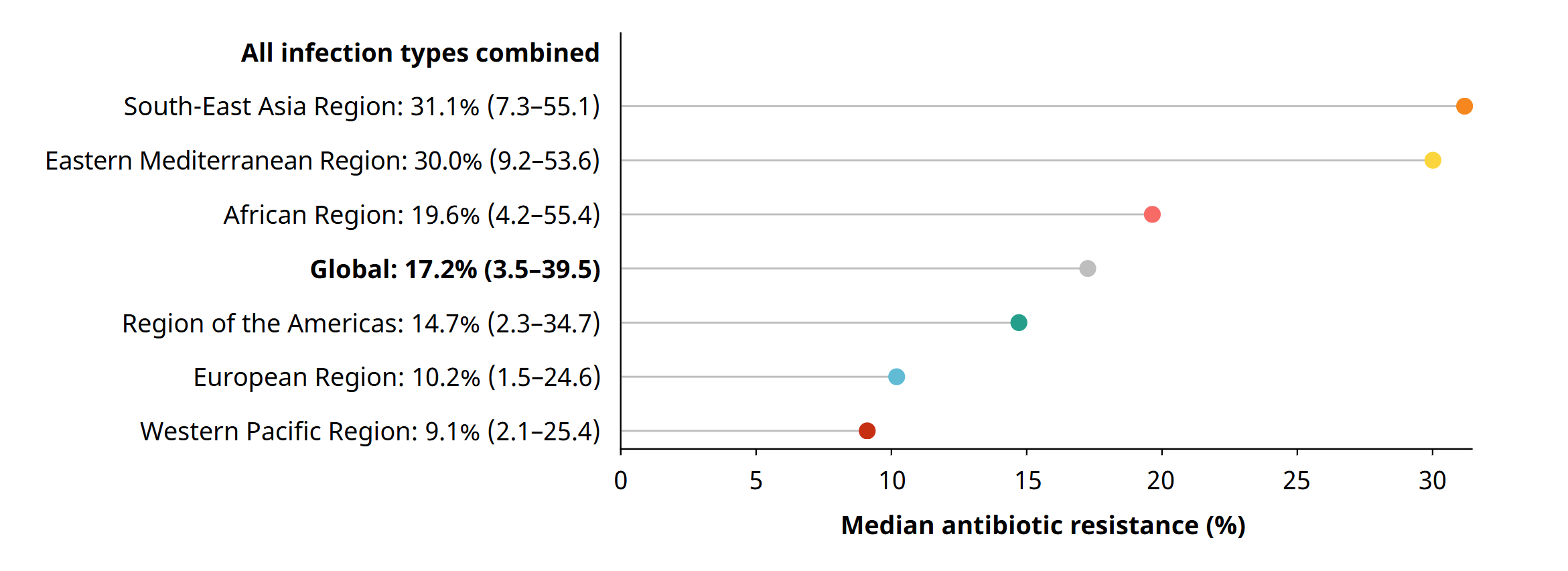
Geographically, the South-East Asia and Eastern Mediterranean regions reported the greatest burden, with nearly one in three infections showing resistance, followed by the African Region, where one in five infections were resistant—both surpassing the global median.
Conversely, resistance was less prevalent in the European Region (one in ten) and lowest in the Western Pacific Region (one in eleven), highlighting marked regional differences.
Median national percentage of AMR in bloodstream infections by AMR surveillance coverage, 2023.
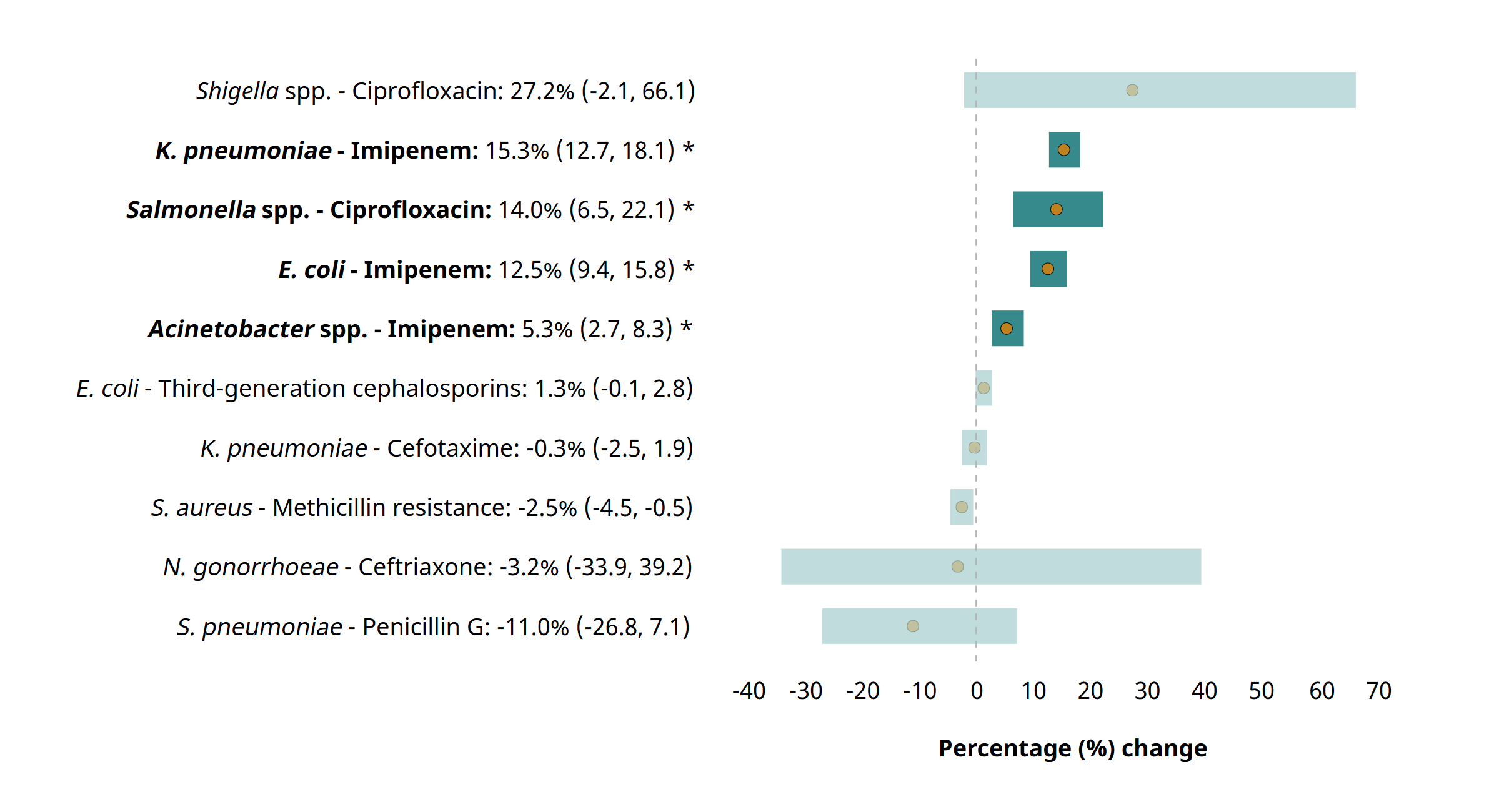
Between 2018 and 2023, antimicrobial resistance (AMR) has risen in 40% of the pathogen–antibiotic combinations tracked for global trends, with annual relative increases ranging from 5% to 15%, depending on the specific combination.
Resistance is notably growing against “Watch” antibiotics in the AWaRe (Access, Watch, Reserve) classification—particularly carbapenems and fluoroquinolones—among major Gram-negative pathogens such as Acinetobacter spp., E. coli, K. pneumoniae, and Salmonella spp.
This trend is concerning because these drugs are critical for treating severe infections. The rise in AMR is narrowing empirical treatment options and prompting a shift from oral to intravenous therapies, with increased dependence on second-line and last-resort antibiotics.
Socioeconomic conditions and the robustness of healthcare systems play a major role in determining the burden of antimicrobial resistance (AMR), with weaker health systems experiencing higher rates of resistance.
Analysis shows a strong inverse relationship between the Universal Health Coverage (UHC) service coverage index—which measures access to essential health services—income level, and the median proportion of AMR in bloodstream infections. This pattern suggests a syndemic, where AMR disproportionately impacts countries with limited healthcare capacity and lower income.

Median national percentage of AMR in bloodstream infections (2023),by income classification and universal health coverage (UHC) service coverage index.
GLOBAL TRENDS
Infections with AST
Here are some representations of numbers of infection episodes with AST results per million population in 2023.

Bloodstream Infections
Here are some representations of the National percentage resistance in bloodstream infections, 2023.
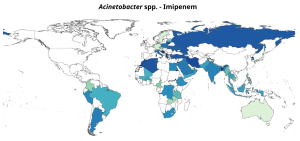
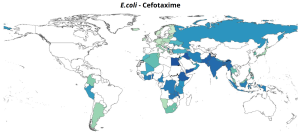
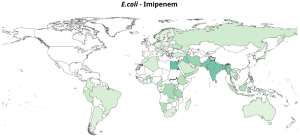
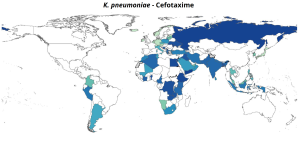
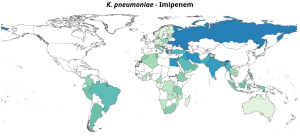




Gastrointestinal Infections
Here are some representations of the National percentage resistance to ciprofloxacin in gastrointestinal infections, 2023.


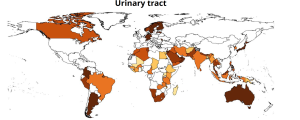
Urinary Tract Infections
Here are some representations of the National percentage resistance to selected antibiotics in urinary tract
infections, 2023.



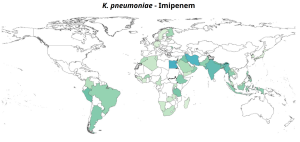
Urogenital Infections
Here are some representations of the Percentage antibiotic resistance to ceftriaxone in N. gonorrhoeae urogenital infections, 2023
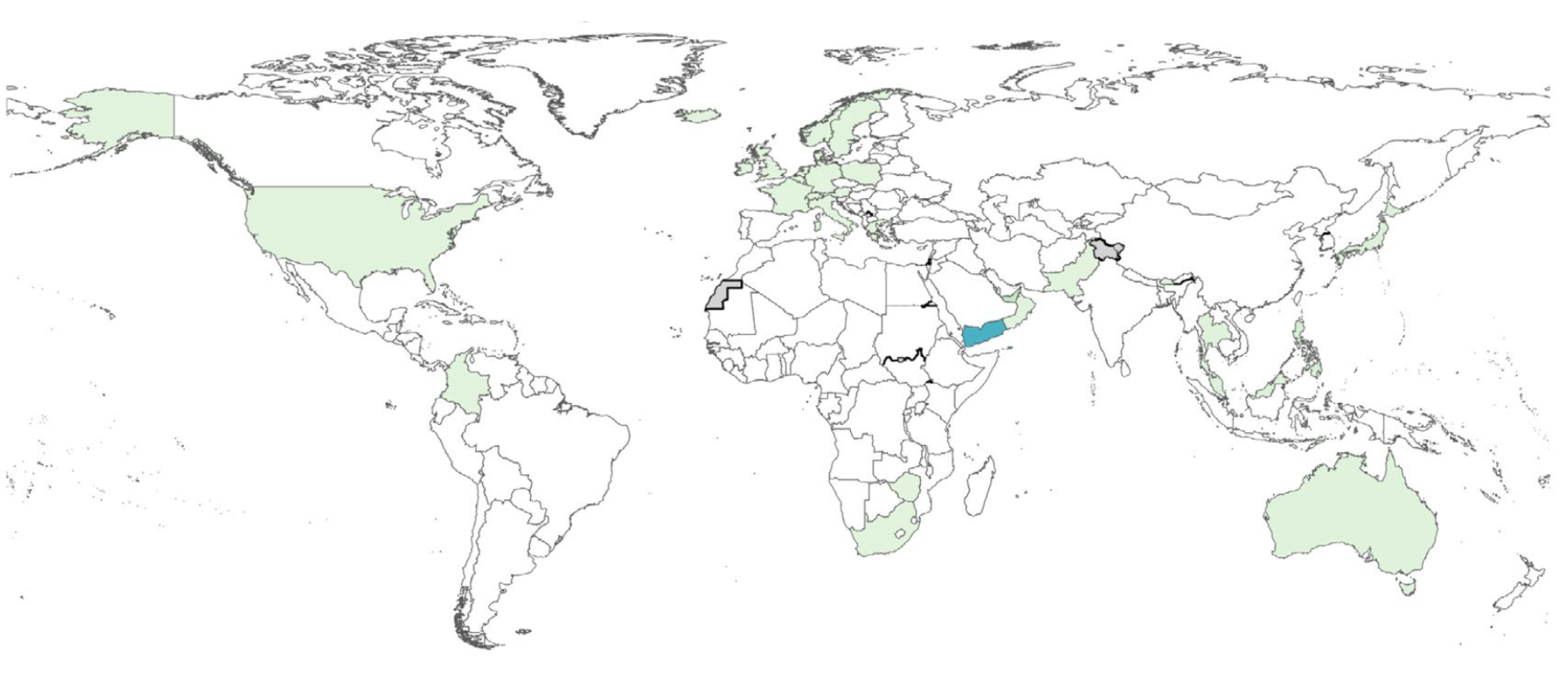
Percentage AMR
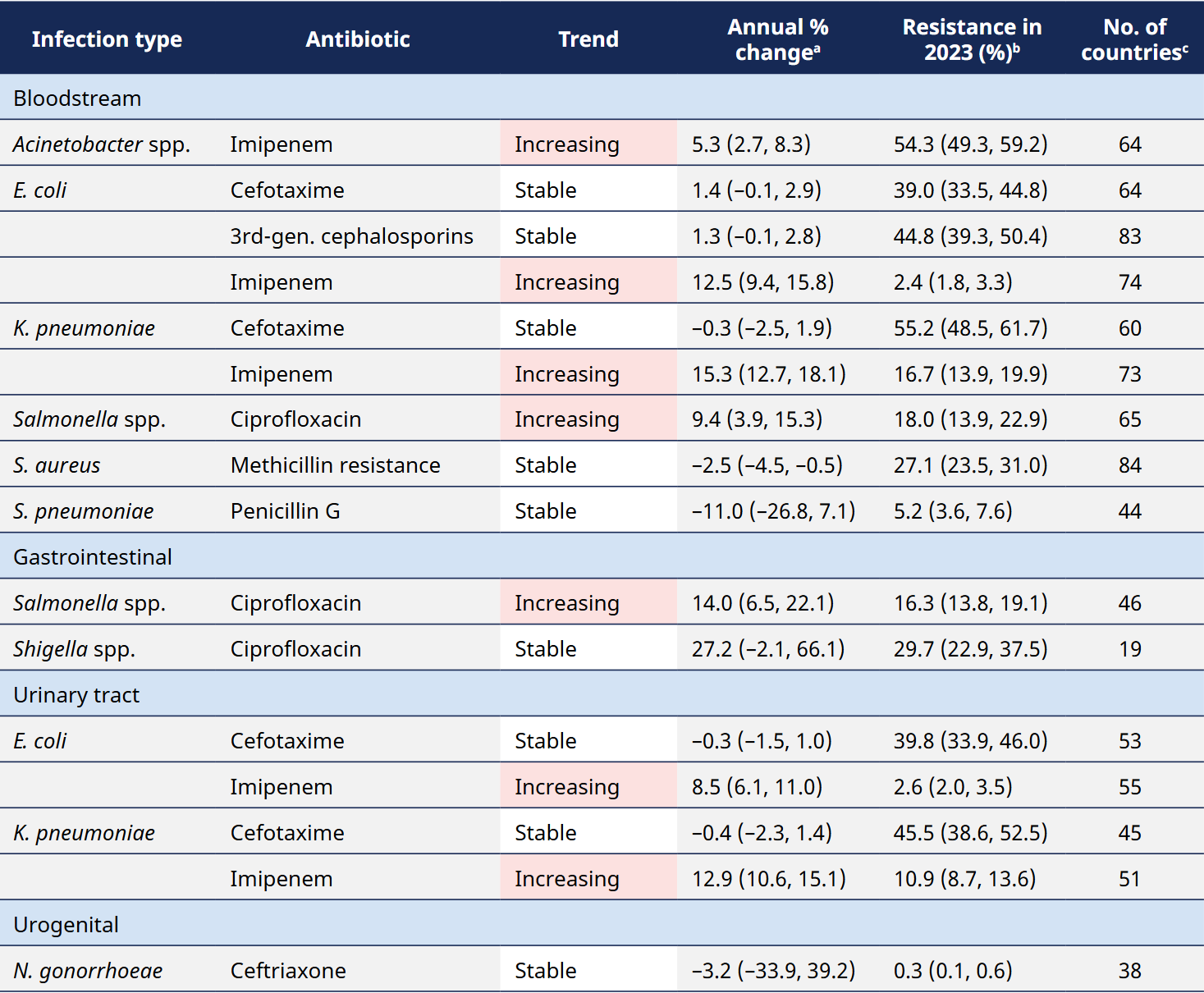
Global trends in percentage AMR by infection type: median annual change (2018–2023) and 2023 percentage resistance estimates :
INDIAN STATS
The numbers below were a part of Global antibiotic resistance surveillance report 2025 :
1
Blood Stream Infections
DRUGS
NO. OF INFECTIONS WITH AST, 2023
NO. OF INFECTIONS WITH AST, 2018-2023
% RESISTANCE
Acinetobacter - Imipenem
9946
30,983
71.2
E. coli - Cefotaxime
6564
25,744
78.5
E. coli - Imipenem
8962
30,295
32.3
E. coli - IIIrd Gen Cephalosporins
6564
17,527
79.4
K. pneumoniae - Cefotaxime
6132
24,864
79.6
K. pneumoniae - Imipenem
9065
32,301
61.2
Salmonella - Ciprofloxacin
-
-
-
S. aureus - Methicillin
8373
37,592
50.9
S. pneumoniae - Penicillin G
-
-
-
2
Gastrointestinal Infections
DRUGS
NO. OF INFECTIONS WITH AST, 2023
NO. OF INFECTIONS WITH AST, 2018-2023
% RESISTANCE
Salmonella - Ciprofloxacin
340
1084
28.9
Shigella - Ciprofloxacin
186
186
82.1
3
Urinary Tract Infections
DRUGS
NO. OF INFECTIONS WITH AST, 2023
NO. OF INFECTIONS WITH AST, 2018-2023
% RESISTANCE
E. coli - Cefotaxime
51,874
174,593
73.5
E. coli - Imipenem
64,488
206,402
19.2
K. pneumoniae - Cefotaxime
13,440
44,535
69.9
K. pneumoniae - Imipenem
18,739
59,460
40.3
4
Urogenital Infections
DRUGS
NO. OF INFECTIONS WITH AST, 2023
NO. OF INFECTIONS WITH AST, 2018-2023
% RESISTANCE
N. gonorrhoea - Ceftriaxone
-
-
-
AMRSN, 2013

Antimicrobial resistance (AMR) represents a significant public health challenge in India, a country with a high prevalence of infectious diseases and extensive, often unregulated, antibiotic use. Accurate assessment of the AMR burden is essential to understand its consequences, while knowledge of local resistance trends is critical for developing both empirical and pathogen-specific treatment strategies suited to varied epidemiological contexts.
In view of this, to generate relevant evidence on the extent of drug resistance and a nationally representative reliable data on AMR which was not existent from India, ICMR initiated Antimicrobial Resistance Surveillance and Research Network (AMRSN) in 2013.
Goals :
- Establish network of hospitals to monitor trends in the antimicrobial susceptibility profile of clinically important bacteria and fungi limited to human health.
- Include comprehensive molecular studies for identifying the clonality of drug-resistant pathogens and their transmission dynamics to enable better understanding of AMR in the Indian context and develop suitable interventions.
- Disseminate information on AMR in pathogenic organisms to stakeholders to promote interventions that reduce AMR.
- Create data management system for data collection and analysis.
Focus :
- Enterobacteriaceae causing sepsis,
- Gram negative non-fermenters,
- Enteric fever pathogens,
- Diarrheagenic bacterial organisms,
- Gram positives: staphylococci and enterococci and
- Fungal pathogens (excluded in WHO priority pathogens)-yeasts (Candida and Cryptococcus spp.) and mycelial fungi (Aspergillus spp. and Zygomycetes spp.)
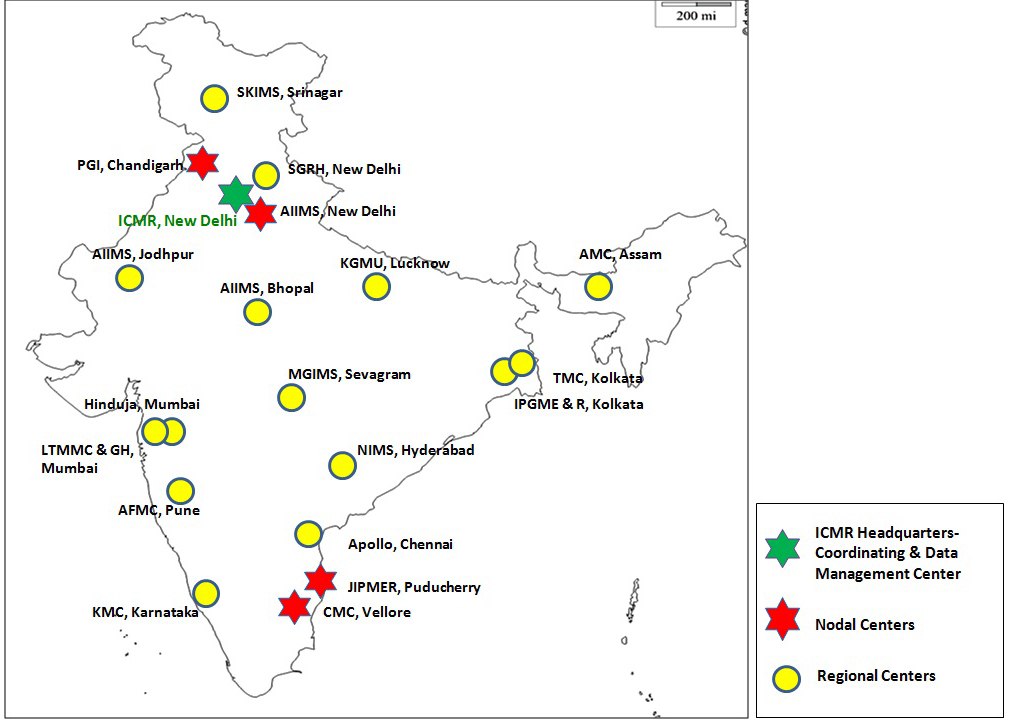
Collaboration with Institutes :
- Diarrheagenic bacterial organisms, CMC, Vellore
- Enteric fever pathogens: AIIMS, New Delhi
- Enterobacteriaceae causing sepsis: PGIMER, Chandigarh
- Gram negative non fermenters: CMC, Vellore
- Gram positives including MRSA: JIPMER, Pondicherry
- Fungal infections: PGIMER, Chandigarh

0 comments