Telemedicine is no longer a futuristic concept, but rather a reality of how people receive healthcare nowadays. In simple terms, telemedicine is the practice of delivering medical services remotely, using technology such as video calls, apps, messaging, and remote‑monitoring devices. That is, one can get expert opinion with only a click now!
The COVID-19 pandemic has significantly accelerated its evolution from a niche “backup option” into a mainstream model of care. It is now being used for routine check-ups, chronic‑disease management, mental‑health counselling, emergency triage, and even remote‑surgical support.
In India, eSanjeevani portal and private‑sector apps are already being promoted and put into use.
Join Weekly Health Newsletter
Every week, I will share with you information about Natural Health, Diet, Exercise, Yoga & Wellness.
WHAT IS TELEMEDICINE?

Many people use “telemedicine” and “telehealth” interchangeably, but :
- Telemedicine refers to clinical services delivered at a distance [like consultations, prescriptions, and follow-ups]
- Telehealth is a broader umbrella comprising of telemedicine, remote monitoring, health‑education courses, and public‑health campaigns delivered through digital channels.
Within telemedicine, there are three main modes:
- Live‑interactive video visits
- Store‑and‑forward: Patients or local clinics send photos, scans, and lab reports to a specialist who reviews them later and issues a report or recommendation
- Remote patient monitoring (RPM): Patients use devices (blood‑pressure cuffs, glucose meters, smartwatches, ECG patches) that transmit data to clinicians, who then track trends and intervene when needed.
In India, telemedicine has been formally guided by the Telemedicine Practice Guidelines (2020), updated in 2026. It requires the doctors to be registered, patient identity to be verified, proper documentation, informed consent, and treatment with the same professional standards as in-person visits.
PATIENT'S BENEFITS
For patients, telemedicine is primarily about access, convenience, and continuity.
- Telemedicine removes geography as a barrier to expertise.
- No long queues, no crowded waiting rooms. Also, greater compliance would be observed in cases of multiple regular follow-ups.
- For Chronic‑disease management, like diabetes, hypertension, heart failure, chronic kidney disease, and autoimmune conditions. It can schedule regular check-ins, track lab results, and watch trends from home devices, helping the patient prevent avoidable hospitalizations.
- Tele‑counselling and tele‑psychiatry let people seek help from the privacy of their homes, reducing stigma and shame
- Post‑treatment and rehabilitation. After surgery, or hospital discharge, patients can receive physiotherapy guidance and nutrition coaching easily.
DOCTORS AND TELEMEDICINE
With a skewed doctor-to-population ratio here in India, telemedicine can provide a structure, thus decreasing OPD crowd, waiting time, and delivery of urgent care.
The following are some possible scenarios:
- Pre‑visit triage: A patient can fill out an online, listing his symptoms, medications, and allergies. This information is then forwarded to the physician before the call starts.
- During the visit: The platform can access the patient’s medical history, lab results.
- Post‑visit automation: After the call, the system can auto‑generate notes, send prescription orders as suggested, schedule follow-up reminders, and flag patients with notifiable diseases.
REGULATIONS, PRIVACY AND ETHICS
Because telemedicine deals with highly sensitive health data, it sits at the intersection of law, ethics, and technology.
- In India, the 2026‑updated Telemedicine Practice Guidelines stress that the same professional standards apply whether care is given in‑person or remotely.
- Patients must be clearly informed about how their data are stored, who can access it, and how long records are kept. Teleconsultation records must be as complete and secure as physical‑chart notes.
- End-to-end encryption is a must, for maintaining patient’s privacy. Another possibility could be integrating the private telemedicine data into national digital‑health platforms such as India’s Ayushman Bharat Digital Mission (ABDM).

Telemedicine Practice Guidelines, India
- Strict scrutiny over AI-generated results should be kept. Confirming the result with a physician could be one step towards it.
TELEMEDICINE IMPLEMENTATION GUIDE BY WHO

CASE STUDY: eSANJEEVANI

Launched in 2018 by the Ministry of Health & Family Welfare, Government of India, eSanjeevani is a cloud-based national telemedicine platform developed by C-DAC, Mohali. It was integrated with Ayushman Bharat Health & Wellness Centres (HWCs).

Objectives
Its main objectives were to:
- Address shortage of doctors and specialists at primary level
- Reduce burden on district and tertiary hospitals
- Create electronic health records and ensure continuity of care
During COVID-19 lockdown (when OPDs were closed), it was expanded into eSanjeevaniOPD, a free patient-to-doctor teleconsultation service for all citizens.
Parts of eSanjeevani
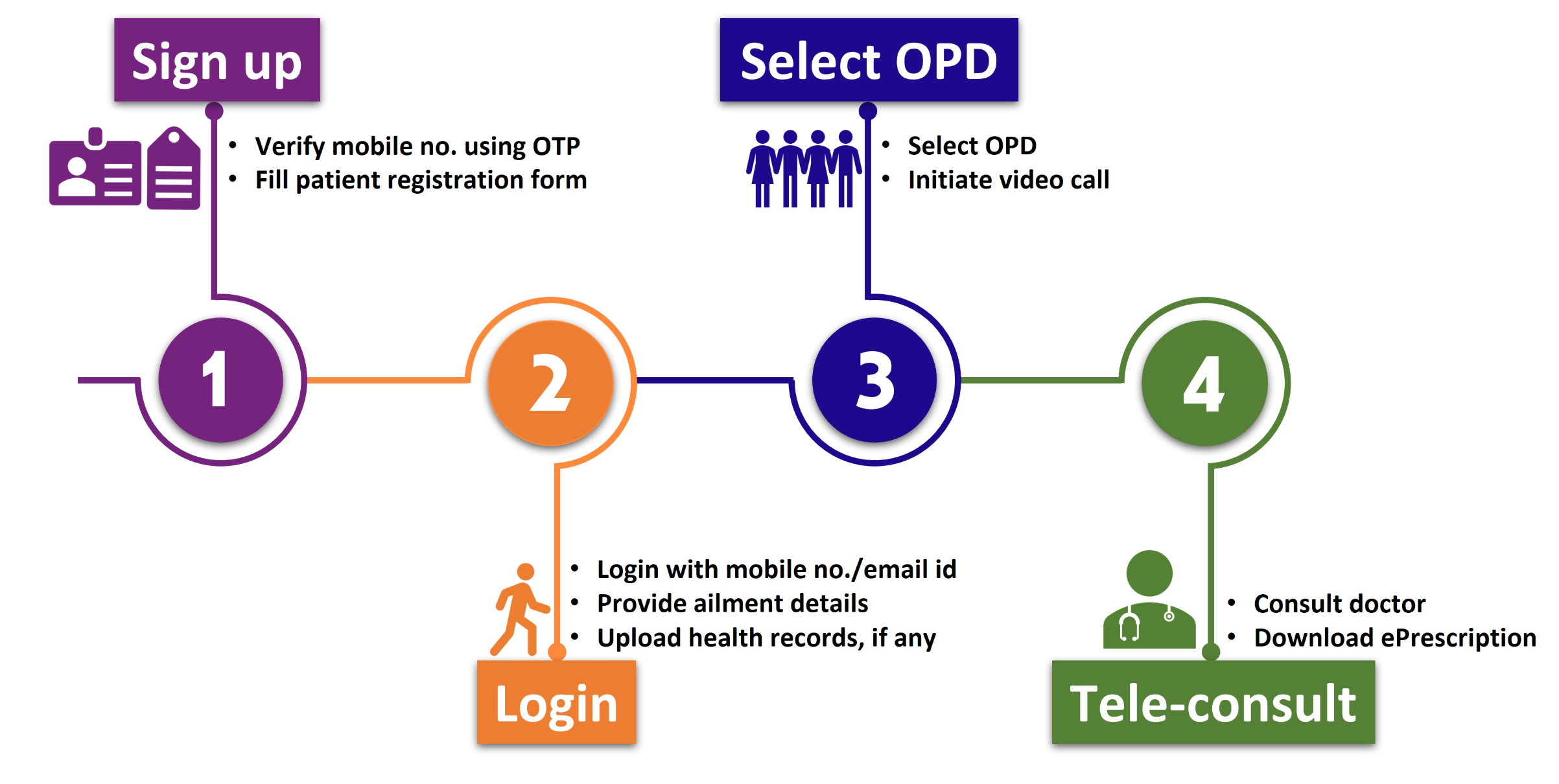
Patient to Doctor Telemedicine
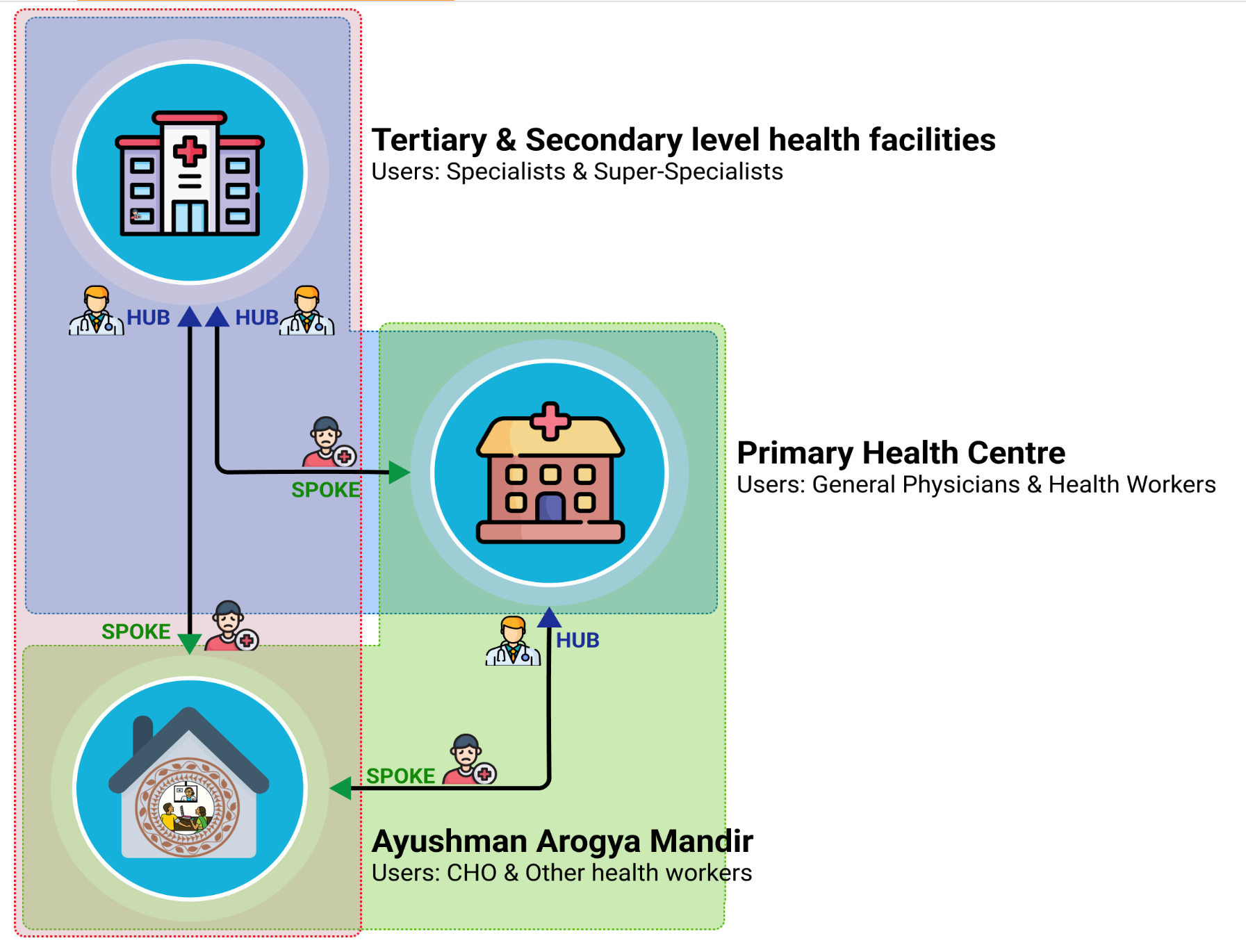
Assisted Telemedicine
It has two components :
- eSanjeevaniHWC (Hub-and-Spoke Model)
- Health worker to doctor teleconsultation
- Used at rural HWCs
- EMR created → patient connected to doctor → ePrescription issued → medicines dispensed locally
- eSanjeevaniOPD
- Direct patient-to-doctor consultation via web/mobile app
- Patient registers → receives token → waits in virtual queue → doctor consults → prescription issued
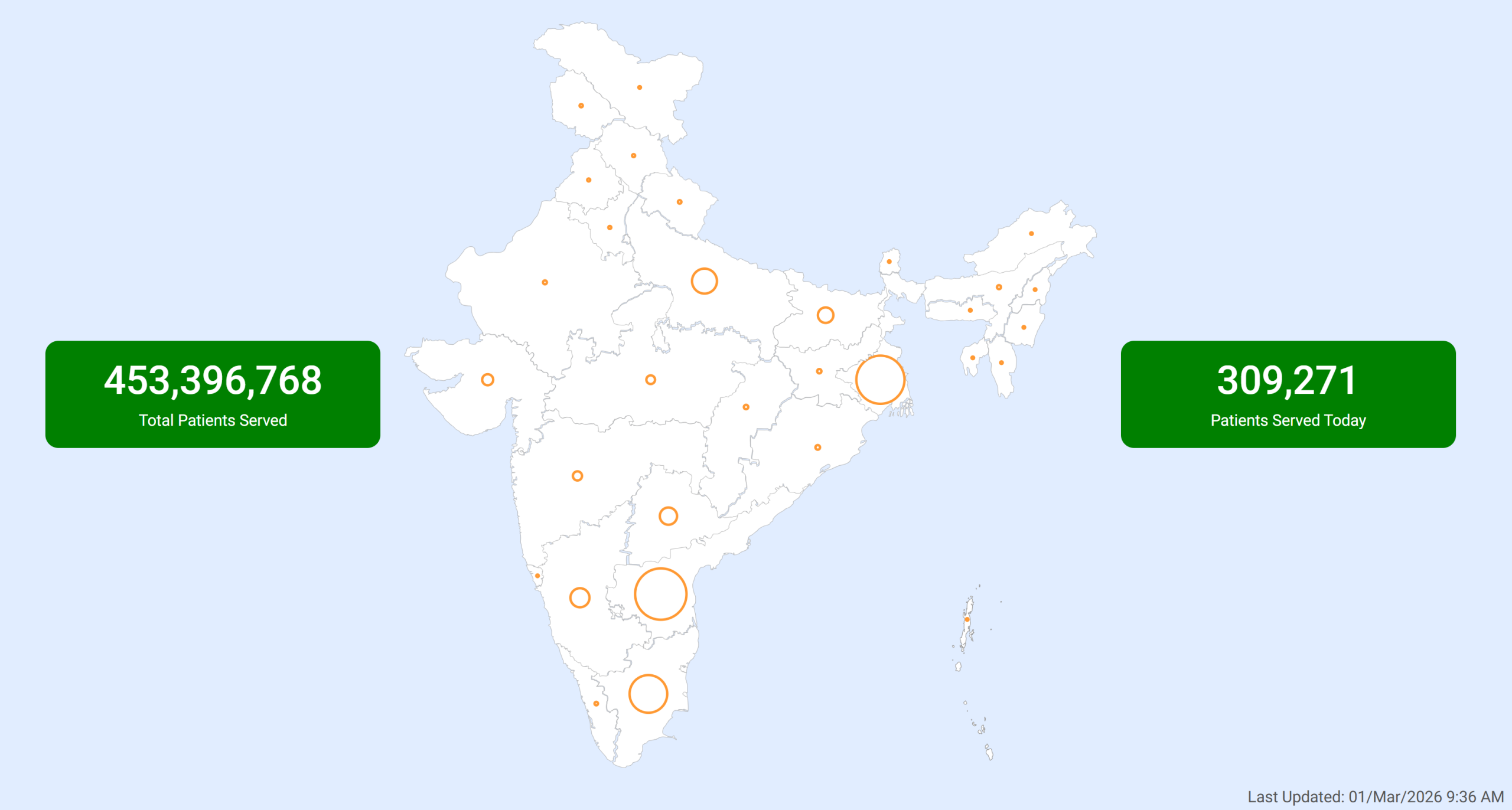
Issues Faced
- Scaling issues
- No SOPs initially [Standard Operating Procedures]
- Digital illiteracy among health workers
- Low public trust in telemedicine
- Demand spikes
Their Solutions
- Shifted to hyperscale cloud system
- Developed and revised SOPs with MoHFW
- Extensive training & trial sessions
- Awareness campaigns & user guides
- Continuous monitoring & forecasting
Lessons & Future Plans
- Higher internet penetration increased usage, but demand was strong even in low-connectivity and remote areas.
- Strong local technical support ensured 99.5% uptime.
- Integrated with Ayushman Bharat Digital Mission for health records linkage.
- Expanding to eSanjeevani 2.0 with AI features, multilingual interface, and capacity for 1 million consultations/day.

CHALLENGES AND LIMITATIONS
Despite having positive effects on the current healthcare infrastructure, it comes along with some challenges.
- Digital divide: People may lack stable internet, smartphones, or the digital literacy to use apps.
- Physical‑exam limitations: Conditions like acute abdominal pain, complex injuries, and certain surgical cases would still require in-person exams, palpation, or imaging that cannot be fully replicated remotely.
- Privacy and commercialization risks: Breaches, misuse of data, or aggressive marketing practices can erode patient trust too.
THE FUTURE OF TELEMEDICINE
- Instead of “in‑person vs. telemedicine,” the future is hybrid care—mixing face‑to‑face visits, video consults, phone calls, and remote monitoring based on each patient’s needs and condition.
- As smartwatches, continuous glucose monitors, ECG patches, and implantable devices become more accurate and affordable, telemedicine dashboards will receive richer, real-time data streams, thus enabling earlier intervention.
- Telemedicine will be a key tool for delivering specialist care in low‑resource and remote regions, including tribal belts and underserved districts of India, where building enough hospitals and training enough specialists in‑person is physically and financially challenging.
REFERENCES
Consolidated telemedicine implementation guide. 9 November 2022 Publication. ISBN: 978 92 4 005918 4
eSanjeevani, National Telemedicine Service. Link.

0 comments